Managing changes to memory and thinking
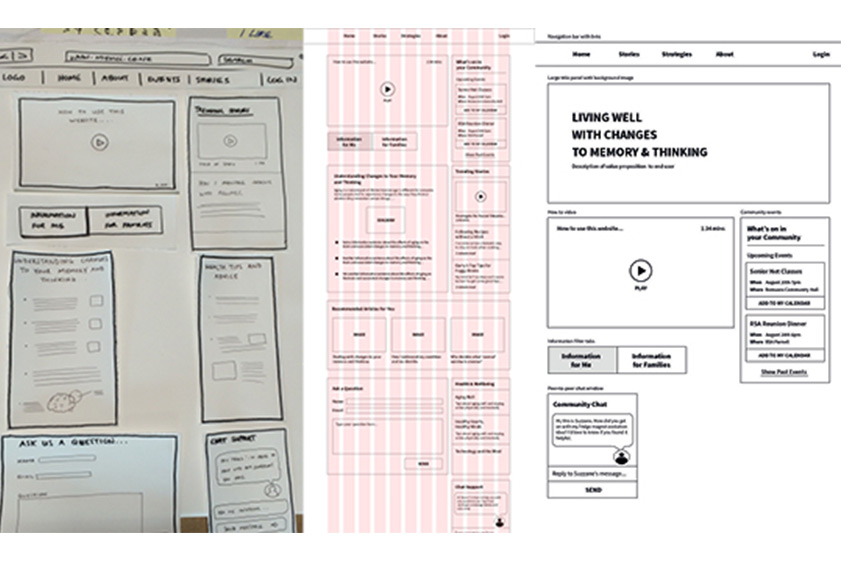
Developing a web resource where users can share stories about, and strategies for managing, changes to their memory and thinking.
Links and downloads
- You can check out the website here: http://www.greymatters.co.nz/
- You can download an A4 poster to promote the website to your community
- You can download a postcard to give to your client/member and their family members
- For professional print files of these materials you can download the poster and postcards A4 or A6, or contact us
Project background
The overarching goal of this project was to co-design an interactive website resource with and for people experiencing changes to their memory and thinking.
Where did we start?
While much is known about deficits in functioning caused by mild cognitive impairment (MCI), much less is known about how people live with the condition, the strategies and supports people find most helpful, and the language they use to describe their experience. Given this, Professor Kathryn McPherson had the idea that we could do a piece of work where we could get to know and understand peoples experiences and perspectives, and work with them to develop a website resource to share with others like them. We hoped this website could be an interactive resource where people could contribute stories over time. The vision was that we could then draw on this living resource to embed the perspectives of people with MCI into the ongoing work of Brain Research New Zealand (http://www.brnz.ac.nz/) so that their research could be underpinned by the needs and concerns of people with lived experience.
Soon after securing funding from Brain Research NZ for this project, Professor McPherson moved on from Auckland University of Technology. It was at this time that Professor Nicola Kayes took leadership of this project alongside University of Otago colleagues, Professor Pauline Norris and Professor Leigh Hale.
What did we do?
We worked through a range of key phases starting with in-depth individual interviews with people who self-identified as experiencing changes to their memory and thinking (n=8) or who had been identified by their medical practitioner as having MCI (n=11) and their family members (n=9).
In the interviews, we were struck by the deep sense of uncertainty people experienced. People we spoke to navigated this by both ‘sense-making’ and ‘meaning-making’.
Navigation processes
‘Sense-making’ refers to the process of trying to make sense of one’s experience. This was made more complex by the lack of a clear distinction between ‘normal’ age-related decline and early dementia. A number of things contributed to this sense-making process including: a) the formal processes of assessment and diagnosis, b) available discourses of ageing, memory failure and decline, c) personal narratives and experiences of dementia, d) symptoms and experiences which challenged assumptions of self-continuity, and e) cultural interpretations.
- “It’s hard to tell with some of these little things whether it’s a natural ageing process or…. something more sinister”
- “My father and his mother both had Alzheimers. I’m concerned I…. you know… I don’t know whether there’s a familial thing there or not, but gee, all of a sudden, heck, I need to know if this could be a precursor.”
- “If any such diagnosis does happen, from my point of view, what would be really useful is to actually understand more about it. What we need to, what we have to expect going forward, and because… you know… because as non-medical people, we don’t really understand”
‘Meaning-making’ refers to the process of trying to understand the implications now and into the future. Participants stories were primarily centred on a) the impact on sense of self and identity (i.e. where usual markers of productivity, success and contribution were under threat), and b) impact on a possible future (i.e. where the uncertain and unstable reality they found themselves in impacted on future possibilities). Participant’s interpretations tended to be heavily influenced by their ‘sense-making’ processes – with contrasting, and sometimes co-existing, experiences of fear and anxiety versus perceived control and hope for the future.
- “Yeah, that’s one of the worst effects of the whole thing, getting frustrated not being able to do things that you feel convinced yourself that you should be able to do”
- “The scary part is to realise that I am experiencing some changes in my cognitive skills and I always relied on them tremendously, like hands and feet, you know?”
- “I have always been independent and self-sufficient and… now it’s a little bit scary at this stage and age, whoa […] I’m not able to do some of the things that I have always been able to do to, to rely on myself and do”
Who were we designing for?
The stories of our interview participants really highlighted the blurry edges of an MCI diagnosis. It was difficult for people to distinguish if their experiences were ‘normal’ age-related decline, or a sign of something more. Even those who had been identified by a medical practitioner as having MCI, did not necessary recognise the label or understand what it could mean. Despite seeking certainty, most found that the diagnosis did not give them certainty. If anything, it made them feel even more uncertain and worried about the future. Many people also commented that if a website were to be developed, it would have been something they would have looked for before accessing formal health services – before they had come to know about MCI as a category.
So, we had to ask ourselves – if we are not designing for ‘people with MCI’, who are we designing for?
In the end we agreed – we were designing for people experiencing changes to their memory and thinking, whether they have been identified to have MCI or not.
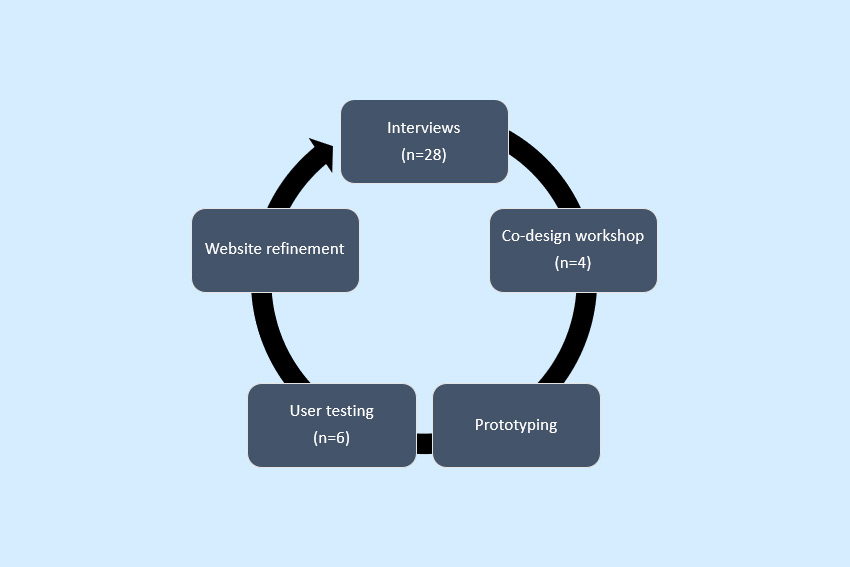
What was our co-design process?
Our co-design process involved multiple steps including:
- A co-design workshop with people experiencing changes to their memory and thinking and their family
- Developing wireframes and prototyping
- Working with participants to prioritise content options
- Building content from the interview data
- User testing to explore acceptability of content, functionality, usability, and look
What we learnt through each of these activities enabled us to further refine the website.
We also worked with some of our AUT design students to develop an animation about MCI to help people make sense of what that might mean as a category for people living with changes to their memory and thinking.
Further details
Conference and other presentations
- Kayes, N. Pauline Norris, Leigh Hale, Guy Collier, Nick Hayes, Project steering group: Richard Worrall, Stephen Reay, Kathy Peri, Suzie Mudge, Duncan Babbage. Co-designing an interactive website resource: a space to share stories and strategies for people experiencing changes to their memory and thinking.
- Collier, G., Kayes, N., Hale, L., Norris, P., Peri, K., Babbage, D., Worrall, R., Reay, S., Hayes, N. (2016, November 24 – 26). Living Well with Mild Cognitive Impairment: Designing an Interactive Online Resource. Paper presented at New Zealand Applied Neuroscience Conference, Auckland, NZ. Neuroepidemiology 47, 132. DOI 10.1159/000453097.
- Collier, G., Hayes, N., Kayes, N., Hale, L., Norris, P., Peri, K., Babbage, D., Worrall, R., Reay, S. (2017, February 17). Designing for Mild Cognitive Impairment: How can design support people experiencing changes to their memory and thinking? Designing for the Ageing Brain Symposium. Auckland, NZ.
- Collier, G., Kayes, N., Norris, P., Hale, L., Mudge, S., Peri, K., Babbage, D., Worrall, R., Reay, S. Hayes, N. (2017, April 26 – 27). Living Well with Mild Cognitive Impairment: How can design support people experiencing changes to their memory and thinking? Poster session presented at BRNZ/MedTech Symposium. Auckland, NZ.
- Collier, G., Hayes, N., Norris, P., Hale, L., Peri, K., Mudge, S., Babbage, D., Worrall, R., Reay, S., Kayes, N. (2017, September 8 – 10). ‘Feeling Like a Ghost’: Insights developed through a co-design approach. Oral presentation at New Zealand Rehabilitation Conference: Making an Impact. Christchurch, NZ.
PhD thesis
Guy Collier, PhD (2020). Getting Old and Forgetting Things: Design anthropology and the medicalisation of mild cognitive impairment (MCI)
https://openrepository.aut.ac.nz/handle/10292/13261
Project details
Funder:
Brain Research New Zealand (BRNZ)
Principal investigator:
Prof Nicola Kayes (Originating PI: Prof Kathryn McPherson)
Research team
Nicola Kayes, Pauline Norris, Leigh Hale, Guy Collier
Contact:
Nicola Kayes
Key Collaborators:
Stephen Reay, Nick Hayes, Richard Worrall, Suzie Mudge, Duncan Babbage, Kathy Peri, Cassie Khoo
Timeline:
January 2015 – January 2020




